Structural or Functional? – Decreased ROM
There have been lots of AHA moments in my life and career. One was when I started looking at ROM as with Structural or Functional. What I mean by this is that when you are testing a joint or movement you need to differentiate between whether what you are seeing is as a result of the patients anatomy, or as a result of their functional capacity.
This is pretty vital!! Not a lot of point in trying to increase the range of a joint that already has its full ROM available. Also, not much point in spending ages trying to increase the ROM at a joint that doesn’t even have the functional capacity to use it!!
You see this sort of thing all of the time. Patients with loads of range when you test passive movements on the physio bed that can’t use it to lunge, squat, go down stairs, etc.
So, How can you tell?
As part of most assessments you’ll be getting hands on and doing passive ROM (PROM), which gives you an idea of what the joint can do with no real demands placed on it.
Let’s use hip flexion as a quick example. In supine take the hip through range and see what you get. you can look with knee straight/bent, you can look at combined movements, etc…At this point, I’m not worrying about what is limiting PROM…but you do get a feel for that too.
Then get them on their feet. Complete squats, lunges or what ever you need to see for their pain, dysfunction or goals. Compare what you see to what you felt. It’s about putting the different elements together to work out where the limitation is.
Structural or Functional at the Foot and Ankle
I think the area of the body that probably triggered this thought process was at the foot and ankle. If you look at the ROM at the ankle in a double squat and then compare it to a single leg squat or a single leg squat with toe touch.
If they can achieve the same ROM at the ankle with DL and SL squats then I’m likely to start looking elsewhere. However, it’s really common to see lots more range DL than SL. My thought here is that the ankle clearly has the range, but can only utilise it when there is lots of stability. You can change the stability by letting them hold on to something or use a stick…then you’ll see the ROM increase again.
This to me says it’s a functional deficit. Now whether it is a strength issue, a coordination issue or a combination of different factors is yet to be determined…but at least now you won’t spend ages working on ankle ROM and wondering why they aren’t improving!!!
If like in some cases there is an underlying issue, like a forefoot equinus…
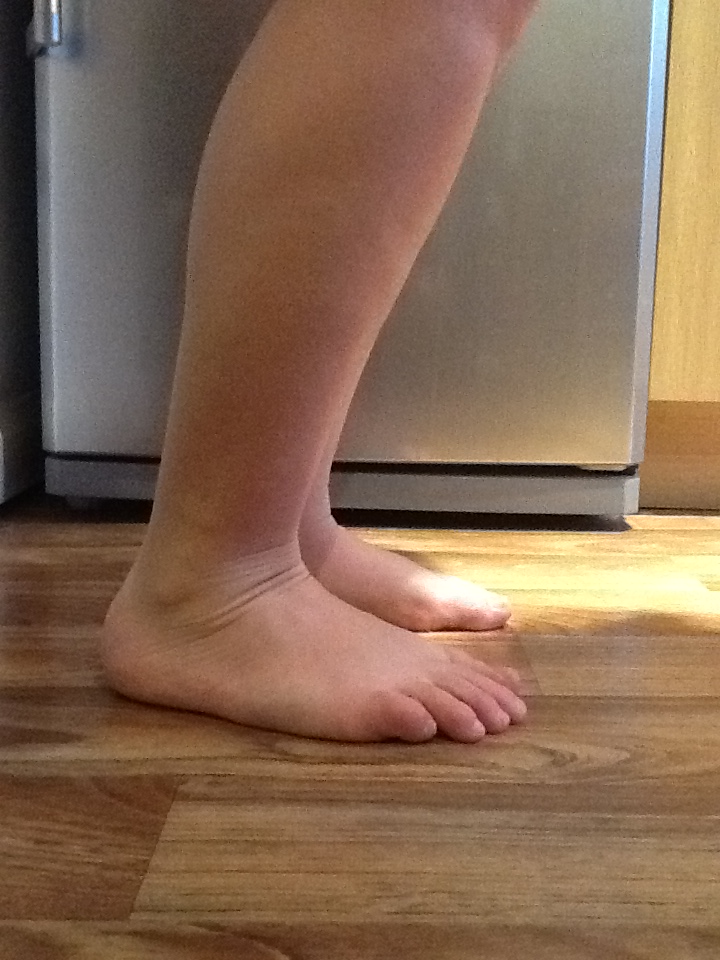
If you ask the above patient to squat DL or SL…there will never be much range. You may work on strength and stability here as much as you want, but it isn’t likely to change anything. You can work a little on joint mobility, but results will be limited. In this case you will be looking at the function around it to get the best result.
This is a massive topic…I think I underestimated it myself here. I’ll try and get a couple of examples in to some posts in the next couple of weeks. It just goes to show how complex assessing movement and function can be!
Physioblogger

