Joint Relationships
When teaching the Physioblogger CPD course it is always really good to get through all of the principles of function and how we apply those in functional assessment and treatment. One of the ones we talk about is ‘joint relationships’. It seems obvious to say that joints are in a relationship with each other, but you would be surprised how many people argue with me that, for example, what is happening at the foot can’t affect the shoulder.
I think part of the problem is that in order to learn anatomy we start to by breaking the body down…this is a muscle, ligament, bone etc and then this is a foot, this is a knee, this is a hip, etc. Though it is probably the best way to get started in anatomy, with all the pressures on the therapy curriculum there is less and less time to take that segmented knowledge and put it together. I think when I was training we had two 2 hour lectures and two 2 hour seminars a week on anatomy for the first year of the course. Personally, I don’t think that’s a massive amount, but it gave us a foundation to build on. As I understand it now the course has squeezed anatomy even more and there is now even less teaching time available.
The big problem with this is that it is very hard to teach/learn anatomy in that amount of time. You can get through all the major structures, but it gives very little time to explore their relationships with each other. The problem this leaves the practitioner with is that it is very hard to bring this segmented knowledge of anatomy into an understanding of functional movement. This is a BIG problem!! As therapists we are dealing with dynamic bodies and when you are practising and learning at the same time it is not always easy to take the anatomy knowledge and turning it into functional anatomy.
For this reason, one of the key principles of function we talk about on the course is joint relationships. We use some practical example to demonstrate the relationships. Testing ranges of motion, altering the position of distant joints and re-testing gives you a great insight into the relationships. Understanding joint relationships has many benefits, particularly in terms of assessment and treatment using function, which is how we use it on the course.
Joint Relationships in Assessment
In assessment the understanding of joint relationships is essential to analyse the movement and function of your patient. I use gait as my main functional basis in practise and on the course. But the wider benefit of the knowledge is that you can analyse any movement, whether it is your patients sporting movement or whether it is something they have to do in their job. When you watch someone move you need to be able to take the movement apart and then build it back together again. Sounds easy, but can be tricky when watching complex movements in sport or even the subtle movements that occur in gait.
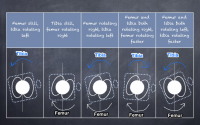
Lets take the example of gait and look at the bone motions in the right leg at heal strike. It’s definitely hard to see the motions in gait, but you can see a few clearly and then your knowledge of relationships helps build the full picture. If we wanted to know what the right hip joint is feeling at heal strike…we can’t really see it clearly, but we can work it out. Assuming we have a ‘normal’ (whatever that is) movement pattern and there are no major dysfunctions, you can clearly see the foot pronating at heal strike and we can see the pelvis rotating to the left…so now we have to fill in the gaps.
If the foot is pronating, we know that the sub talar joint is pronating, causing in the talus to rotate to the left. Due to the congruency of the talo crural joint we know that if the talus goes to the left to that degree then the tibia and fibula are going to have to rotate left also. If the tib/fib are rotating to the left then the tibia will drive the femur to rotate to the left also, causing the knee to internally rotate, unlocking it and allowing it to flex (another example of joint relationships!).
Now we know that both the pelvis and femur are rotating left, so all we need to do is decide which is moving faster to determine the joint motion of the hip. To decide this we need to take into consideration the driver of the motion (since joint surface shape doesn’t influence this motion dramatically). The driver in this case is the ground reaction force from the foot hitting the floor. As a result the power for the motion is from the ground up, which leads me to believe that the femur will be rotating left faster.
So, the joint motion of the right hip at heal strike will be internal rotation, with both proximal and distal bones rotating to the left, distal faster.
You can apply this process to any joint in any plane and therefore analyse any functional movement…a very powerful tool for any therapist.
Next time we will look at how to use this important principle of function in your treatments.
Joint Relationships in Treatment
On Tuesday we talked about this very important principle of function in assessment. It was supposed to be one post, but the word count was starting to get close to my limit for a post…so I decided to split it into separate assessment and treatment posts. So, today we will look at how we can take advantage of our understanding of joint relationships in our treatment strategies.
Quick Re-Cap
Joints are in a relationship with each other, the motion of one can influence all others and by understanding this we can use the motions we can see e.g. gross foot motion/pelvis motion, to work out the the bone and joint motions we can’t see so easily (e.g. transverse plane knee and hip motion). To see the full Part 1 of this article click here: Principles of Function: Joint Relationships in Assessment.
Joint Relationships in Treatment
There are two main ways I think our knowledge of joint relationships helps us to treat our patients:
Making our exercise and manual therapy more functionally accurate
Helping to choose authentic drivers of our exercise and manual therapy
- Functionally Accurate Treatment
Yesterday we used the example of working out what motion occurred at the right hip at right heel strike in gait. Once you have gone through that process, it’s a relatively simple step to take it a stage further and and make this a treatment. We established during the assessment that the pelvis and femur were both rotating to the left, with the femur rotating left faster. So, the right hip will be feeling internal rotation at right heel strike. In order to treat someones dysfunctional gait with limited right hip internal rotation and increase this motion you may want to closely mimic these motions.
For example, I would start by positioning them appropriately, right foot forward. To start I would simply ask the patient to rock forward and back onto their right foot. This is low stress and almost anyone can do it. The manual therapy strategy then can really add to this by slowing down the left rotation of the pelvis and increasing the left rotation of the femur with your hands. Both of these hands on strategies increase the internal rotation force that the right hip will feel and is extremely accurate from a gait function point of view. - Choosing Authentic Drivers
Functional treatment has to be driven from somewhere, as as a therapist we are only adding the last 10%. Our solution should only be creating 90% of the required motion via the patients movement. This means choosing our drivers is very important and understanding joint relationships helps make this much more straight forward.
For our example we will stick with the hips, as that is what we have been using so far. If we wanted to progress the above example of a right hip internal rotation treatment on, we would have to look at what drives that motion in gait and then replicate it. At right heel strike the driver of right hip internal rotation is the ground reaction force. So the best place to start is with GRF, I usually choose short range lunges from neutral stance or very short range lunges from a right foot forward stance. Both of these give a great starting point for your treatment and allows you to get hands on in a way that can enhance the function of your patient.
Sometimes, the above strategy isn’t suitable, whether that is due to a lack of stability or levels of pain, you need somewhere else to go. If you can’t re-create front leg hip mechanics you can choose to go completely different and change strategy. Or, you could look at internal rotation in a different function, e.g. back leg mechanics in gait. As a back leg in gait you still get right hip internal rotation, but this time both the pelvis and femur are rotating to the right, with the pelvis is going faster.
To re-create this motion you can keep the right leg still and pivot around the leg in the transverse plane with the left leg. This creates a nice hip internal rotation motion, with both pelvis and femur rotating right, pelvis faster. Again, one of the great things about this motion is that you can get hands on and increase the benefit to your patient. In this case, you would simply slow down the right rotation of the femur with your hands to increase the internal rotation force.
Summary
What ever your preferred exercise strategy, if you understand the relationships between the joints you will be at a massive advantage in making the exercise more closely match the function of your patient. You can use this strategy with any movement/function and then build appropriate exercises and manual therapy strategies for the individual standing in front of you.